Clinical cases in vascular techniques
This section provides a selection of clinical cases provided by experts in vascular techniques.
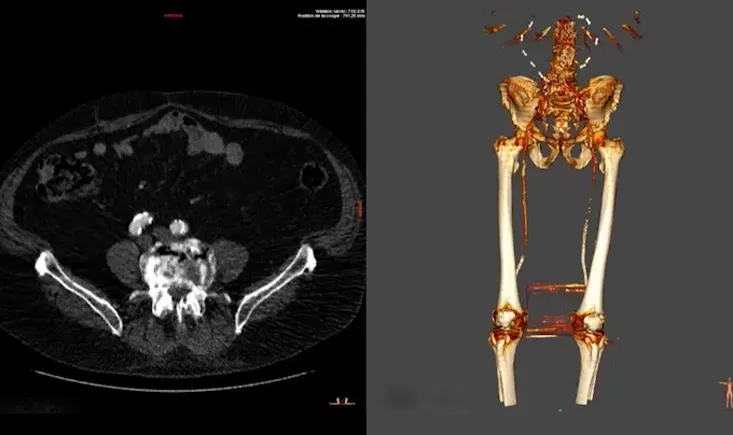
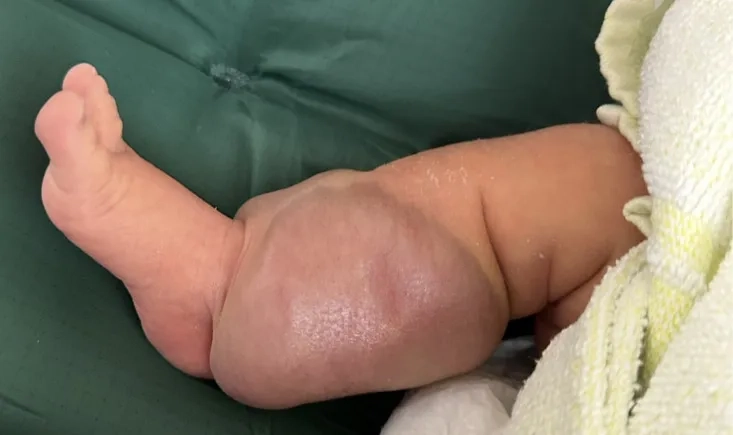
A rare, aggressive AV malformation in a 7-day-old baby, diagnosed as Kaposiform hemangioendothelioma, poses a high risk of rapid growth and severe bleeding. What treatment offers the best chance to control this life-threatening condition?
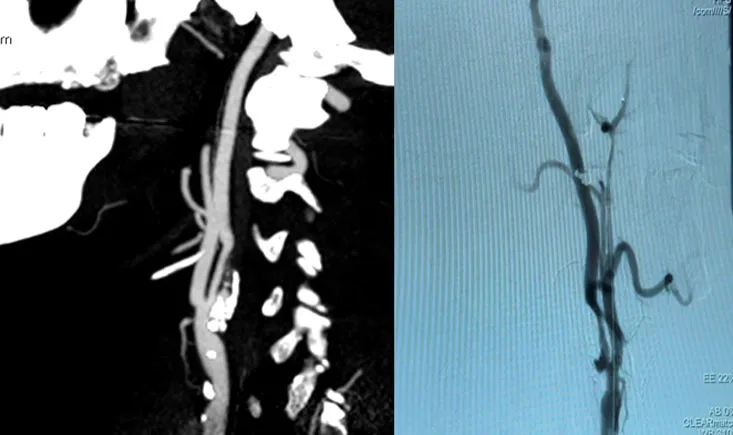
A high-risk 60-year-old male with multiple cardiovascular comorbidities presented with a > 70 % calcified ulcerated stenosis of the left internal carotid artery. Imaging confirmed diffuse parietal disease and a Type I arch. This case explores the therapeutic strategy and technical approach used to manage carotid revascularisation safely and effectively.
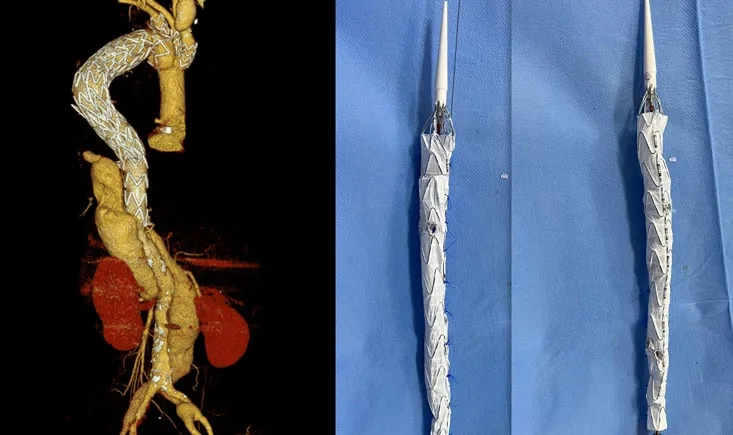
A dissected thoraco-abdominal aorta has evolved into a triple-lumen aneurysm, with two false lumens feeding vital organs and a compressed true lumen in between. This case highlights a staged, fully endovascular repair using physician-modified fenestrations to protect all four visceral branches—avoiding open surgery despite complex anatomy.
A 79-year-old man with diabetes, hypertension, atrial fibrillation, and chronic kidney disease presents with necrosis at the site of a prior toe amputation, performed without revascularisation. TcpO₂ is critically low (3 mmHg), and the WIfI score is 2-3-1. Angiography reveals limited BTK runoff with anterior tibial and peroneal patency, but occlusions of the dorsalis pedis and posterior tibial. Diffuse calcification is observed in foot arteries (MAC-score 5), consistent with a desert foot pattern.
What would be your revascularisation strategy in this challenging scenario?
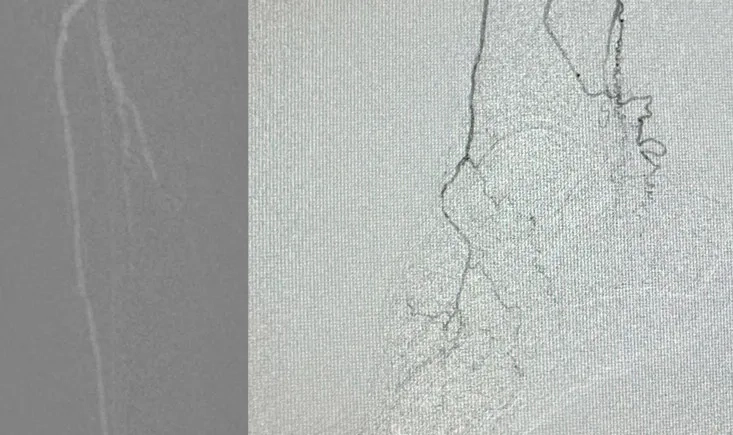
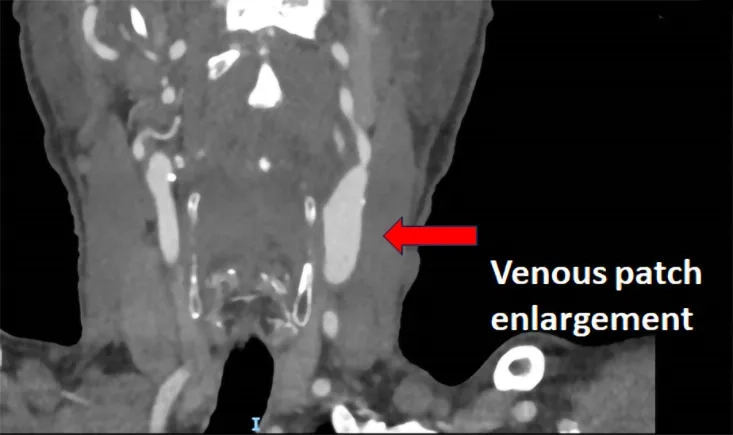
An 80-year-old patient with a complex vascular history presents with left carotid patch enlargement and tight stenosis before the venous patch. With previous strokes and surgical interventions, the case invites discussion on the best management strategy. What would you do next?
This case details a 71-year-old male with a history of AAA and multiple interventions, now facing a large Type II endoleak. Despite several treatments over the years, the endoleak persists, posing a significant challenge. Review the clinical data, imaging, and consider the next steps in treatment through our poll!
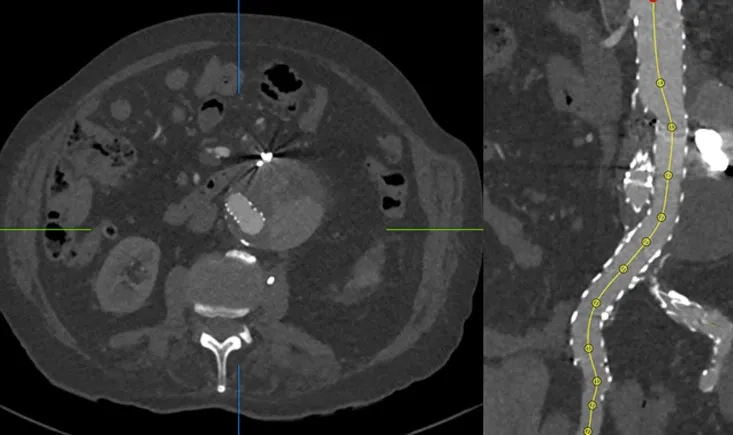
A 69-year-old male with a complex vascular history, including prior stents and endarterectomy, presents with worsening left leg ischemia (Rutherford class IV).
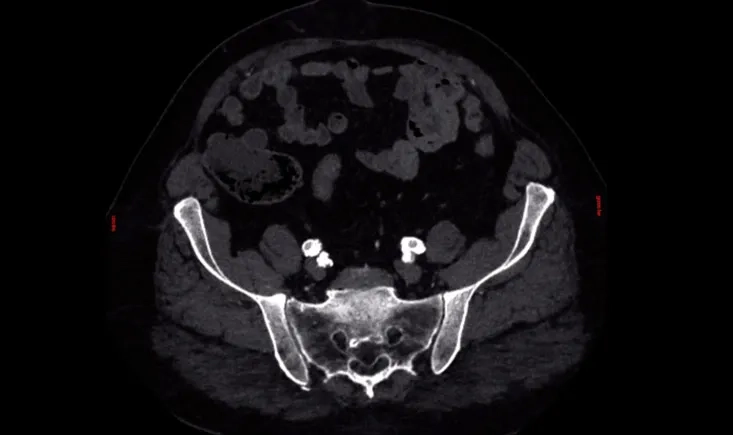
Study the case of a 62-year-old patient with coronary disease, obesity, diabetes, and dyslipidemia, who has a history of RCIA, LCIA, and SFA stenting, along with thromboendarterectomy of the RCFA.
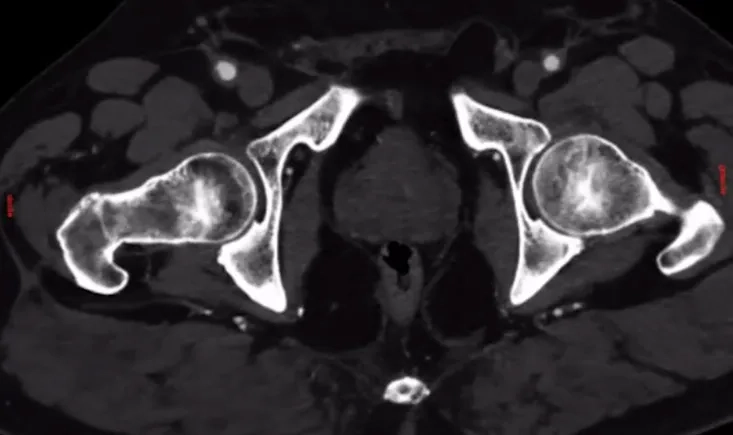
Management of acute limb graft thrombosis can be challenging, especially for an obese patient with Balthazar E severe pancreatitis and ARDS...
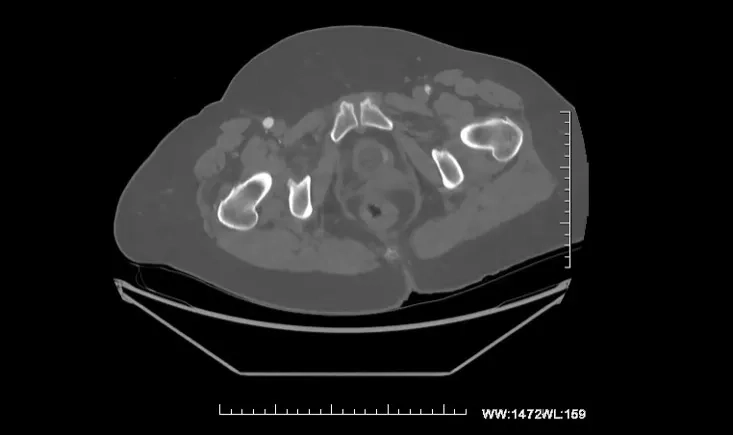
This case was presented at JIF Periph Live on 14 December 2024 by the University Hospital of Bordeaux